The data experts at the Parkland Center for Clinical Innovation in Dallas have developed something they call the "Vulnerability Index." It's a new way to spotlight what ZIP codes in North Texas are most at risk for COVID-19 infections.
One major finding so far: The pandemic is having the harshest impact on communities of color.
KERA's Justin Martin spoke with Steve Miff, president and CEO for the center.
Interview Highlights
On the vulnerability index:
One of the things that we wanted to do is better understand not only COVID-19 and the pandemic, but who is more at risk to not only contacting the disease, but also having more severe symptoms.
So we've taken the literature that's been done and certainly identify four key factors that are significantly contributing to this: age, comorbidities that are associated with COVID-19, social determinants of health and the impact of social deprivation, and mobility.
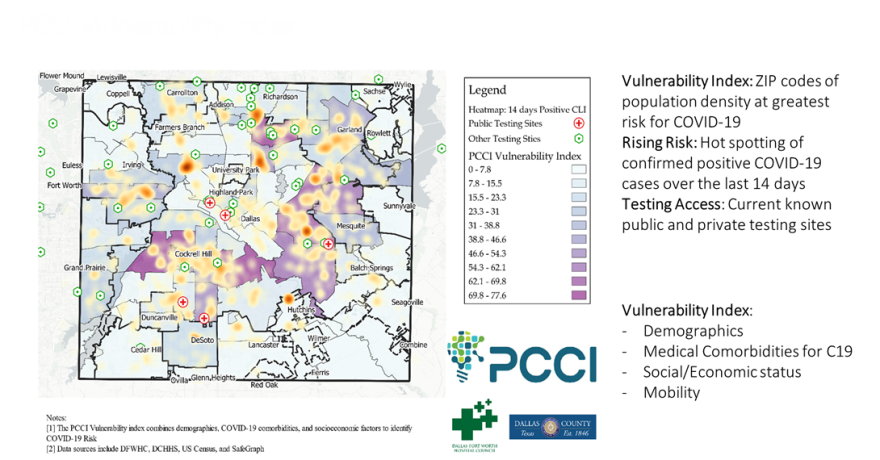
On the maps generated by the index:
So one of the things we've seen is that they certainly match up extremely well with mobility and the ability to lock down. However, they're also significantly important relative to COVID to take into account also comorbidities, because that does put somebody at higher risk, and those while directly linked to social determinants of health.
We also see those very, very strongly correlated to the age of the population.
So it's a multidimensional model, and that's why all these different factors, while by themselves can contribute strongly to predicting which areas are most vulnerable individually, once you bring them all together, that's why we're able to develop this index that has an over 85% correlation to both the positive cases that we've seen across the communities, as well as, again, the COVID-like presentation of illness.
On social deprivation being a leading factor for racial disparities:
Yeah, and there are a lot of different factors that go into that, and they're all related to what we call the social determinants of health.
We know that health doesn't begin in our acute care facilities, but begins in the community where we live, where we work, where we play, where we pray. It's not just one area that is important, it's multiple areas as we think about how do we support our neighbors, how do we support our citizens?
So factors such as access to nutritious food, access to transportation, access to stable housing, being able to afford utilities, elder care, or child care. All those different components is what we mean when we talk about resiliency or social deprivation, and that significantly impact the social determinants of health.
On what this means for communities of color and what hospitials can do about it:
We need to pay particular attention to areas that have populations that are more vulnerable. And that's, again, that's an aggregation of density of people over the age of 65 with comorbidities in areas that have social deprivation. And in some areas they have increased mobility.
So we need to pay particular attention to when we see that rising risk, because that's where there's potential for the disease not only to spread more quickly. But the individuals that contracted the disease to manifest symptoms that require hospitalization or require more intensive care.
By understanding that then the tangible things that we can do is provide proactive and targeted education that is culturally sensitive. I think we need to adapt to who we communicate with in a way that the information makes sense it's being internalized as being received so individuals themselves can do something with that information.
And then number two is deploy both physical testing sites, as well as mobile testing sites in a way they're accessible to individuals in addition to just being able have drive up sites as well.
Interview highlights were edited for clarity and length.
Steve Miff is the President and CEO of the Parkland Center For Clinical Innovation





